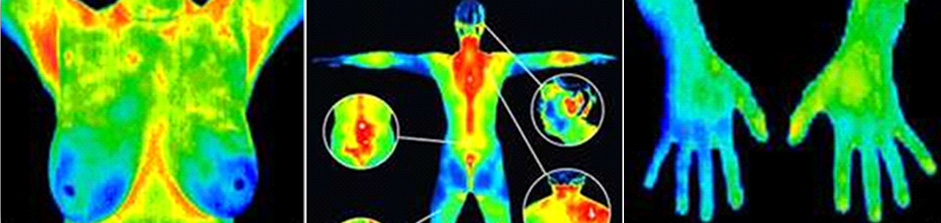
Breast thermography is a 15 minute non invasive test of physiology. It is a valuable procedure for alerting your doctor to changes that can indicate early stage breast disease.
The benefit of breast thermography is that it offers the opportunity of earlier detection of breast disease than has been possible through breast self examination, doctor examination or mammography alone.
Thermography can detect the subtle physiologic changes that accompany breast pathology, whether it is cancer, fibrocystic disease, an infection or a vascular disease. Your doctor can then plan accordingly and lay out a careful program to further diagnose and /or MONITOR you during and after any treatment.
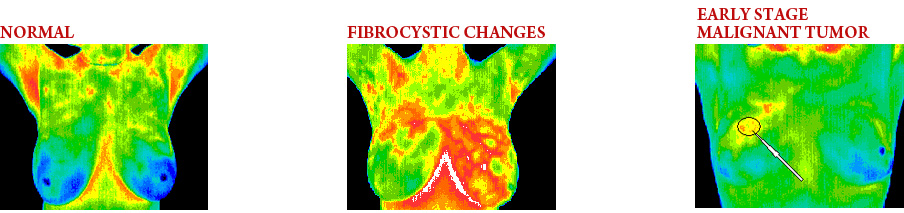
Good thermal symmetry is seen in this picture with no suspicious vascular patterns or significant thermal findings.
The very significant vascular activity in the left breast justified clinical correlation and close monitoring which returned an opinion of fibrocystic changes taking place. These changes can be monitored thermographically at regular intervals until a stable baseline is established and is reliable enough for annual comparison.
This is the specific area of a small DCIS. We can see the vascular feed and the discreet area of hypothermia that is displacing the surrounding hyperthermia.
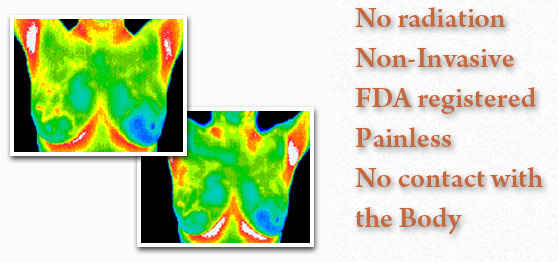
Thermography is a painless, non invasive, state of the art clinical test without any exposure to radiation and is used as part of an early detection program which gives women of all ages the opportunity to increase their chances of detecting breast disease at an early stage. It is particularly useful for women under 50 where mammography is less effective.
Thermography's role in breast cancer and other breast disorders is to help in early detection and monitoring of abnormal physiology and the establishment of risk factors for the development or existence of cancer. When used with other procedures the best possible evaluation of breast health is made.
This test is designed to improve chances for detecting fast-growing, active tumors in the intervals between mammographic screenings or when mammography is not indicated by screening guidelines for women under 50 years of age.
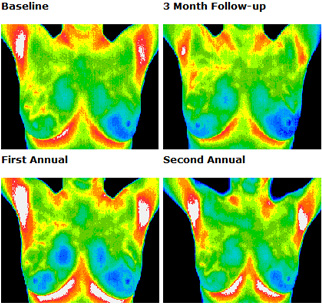
All patients thermograms (breast images) are kept on record and form a baseline for all future routine evaluations.
This patient's thermograms have remained stable for two years. These patterns are like a thermal fingerprint which will only change if pathology develops.
With the new ultra-sensitive, high resolution digital infrared cameras available today, a technology that has been developing over the past 20 years is now becoming more accessible.
Thermography as a physiologic test, demonstrates heat patterns that are strongly indicative of breast abnormality. The test can detect subtle changes in breast temperature that indicate a variety of breast diseases and abnormalities. Once abnormal heat patterns are detected in the breast, follow-up procedures including mammography are necessary to rule out or properly diagnose cancer and a host of other breast diseases such as fibrocystic syndrome, Pagets disease, etc.
By performing thermography years before conventional mammography, a selected patient population at risk can be monitored more carefully. Then by accurately utilizing mammography or ultrasound as soon as is possible, one can detect the actual lesion - (once it has grown large enough and dense enough to be seen on mammographic film), this can increase the patients treatment options and ultimately improve the outcome.
It is in this role that thermography provides its most practical benefit to the general public and to the medical profession. It is certainly an adjunct to the appropriate usage of mammography and not a competitor. In fact, thermography has the ability to identify patients at the highest risk and actually increase the effective usage of mammographic imaging procedures.
Until such time as a cure has been found for this terrible disease, progress must be made in the fields of early detection and risk evaluation coupled with sound clinical decision making.
Thermography, with its non-radiation, non-contact and low-cost basis has been clearly demonstrated to be a valuable and safe early risk marker of breast pathology, and an excellent case management tool for the ongoing monitoring and treatment of breast disease when used under carefully controlled clinical protocols.
